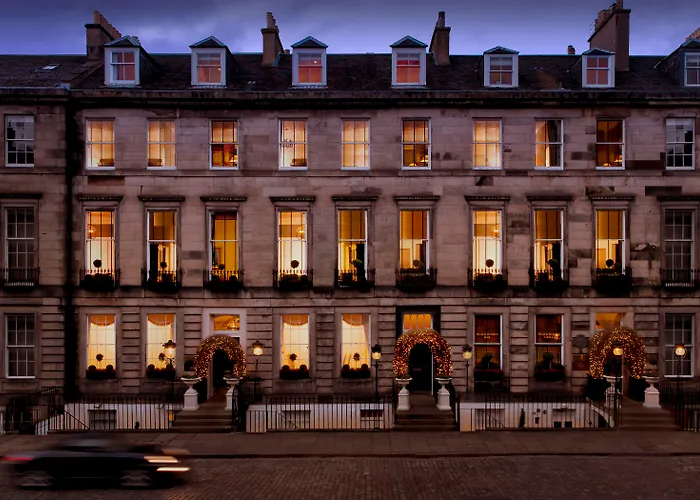Edinburgh Cheap Hotels
The Scots are a thrifty bunch and when it comes to hotels, Edinburgh is no different. There are plenty of cheap hotels in Edinburgh, but why choose them over the more expensive options? Let’s take a look at some of...